Dental Implant Eligibility Checker
Answer the following questions honestly to see if you might be a suitable candidate for dental implants. This tool is for informational purposes only and does not replace professional medical advice.
Your Assessment Result
Verdict:
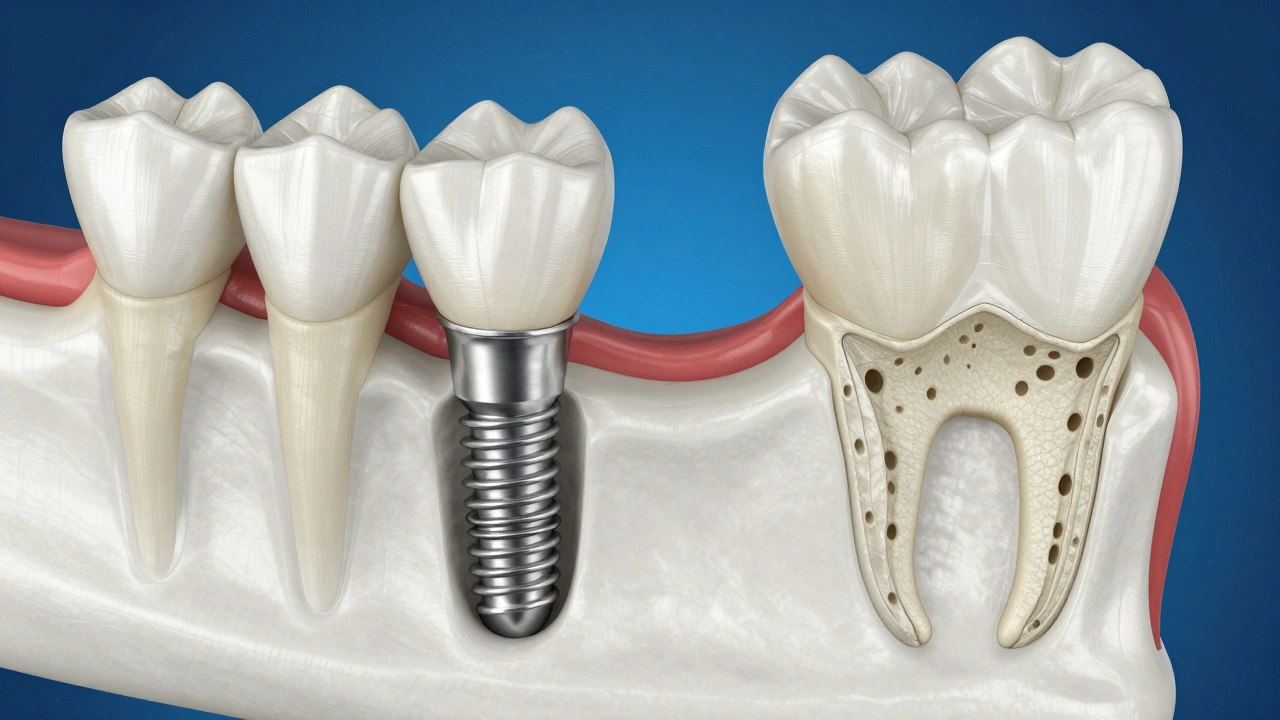
Missing teeth can feel like more than just an aesthetic issue; it affects how you eat, speak, and even your confidence. For many people in the UK, dental implants are titanium posts surgically placed into the jawbone to replace missing tooth roots, serving as anchors for artificial crowns or bridges. They are often called the 'gold standard' of tooth replacement because they mimic natural teeth so closely. However, getting them isn't as simple as booking an appointment and walking out with a new smile. There are strict medical and physical criteria that determine if you are actually a suitable candidate.
If you have been told you might not be eligible, or if you are wondering why your dentist hesitated, understanding the contraindications is crucial. It’s not just about having enough money-though cost is a factor in private care-it’s about whether your body can support the hardware long-term. Here is a clear breakdown of when you should look at alternatives rather than pushing for implants.
The Bone Factor: Why Density Matters
The most common reason people are rejected for dental implants is insufficient bone volume or density. The implant needs to fuse with your jawbone in a process called osseointegration, which is the direct structural and functional connection between living bone and the surface of a load-bearing artificial implant. If your bone is too soft or too thin, the screw will wobble, fail to bond, and eventually fall out.
This usually happens after a tooth has been missing for a long time. When you lose a tooth, the jawbone no longer receives stimulation from chewing, so it starts to resorb (shrink away). This is especially rapid in the upper jaw due to its proximity to the maxillary sinus. If you’ve had a tooth missing for years, you might need a bone graft, which involves a surgical procedure using synthetic material, donor bone, or your own bone to rebuild the jaw structure before implant placement. While grafts can make you eligible, they add months to the timeline and thousands to the cost. In some cases, the bone loss is so severe that even grafting won’t help, making you ineligible for traditional implants.
Uncontrolled Diabetes and Healing Risks
Your blood sugar levels play a massive role in how well you heal from surgery. Type 2 diabetes, if uncontrolled with high HbA1c levels, significantly impairs your body’s ability to fight infection and repair tissue. High glucose levels reduce blood flow to the gums and jaw, slowing down osseointegration.
In the UK, dentists typically look at your HbA1c results. If your levels are consistently above 8% (64 mmol/mol), most surgeons will decline to place implants until your condition is stabilized. This isn't a permanent ban; once your diabetes is managed through diet, medication, or insulin, you may become a candidate again. But attempting surgery while uncontrolled risks peri-implantitis-a severe gum disease around the implant that leads to failure.
The Smoking Barrier
If you smoke, you are already facing a steep uphill battle. Nicotine constricts blood vessels, reducing the oxygen supply needed for healing. Studies show that smokers are twice as likely to experience implant failure compared to non-smokers. The risk of infection and bone loss is significantly higher.
Most reputable dental clinics in the UK will require you to quit smoking for at least two weeks before surgery and continue abstaining for several weeks after. Some surgeons insist on a complete cessation plan. If you are unwilling or unable to stop smoking, you are generally considered a poor candidate. The investment in implants could be wasted if the hardware fails due to lifestyle factors you refuse to change.
Autoimmune Diseases and Medications
Certain autoimmune conditions, such as rheumatoid arthritis, an inflammatory disorder affecting joints that can also impact oral health and healing capacity, or lupus, can complicate implant success. These conditions often involve chronic inflammation that interferes with bone healing.
More critically, the medications used to treat these conditions can be a dealbreaker. Bisphosphonates, drugs used to treat osteoporosis and cancer-related bone loss, carry a rare but serious risk of osteonecrosis of the jaw, which is a condition where the jawbone fails to heal after minor trauma, leading to exposed bone and severe pain. If you take these drugs intravenously, implants are usually contraindicated. Oral bisphosphonates present a lower risk, but your surgeon will need to consult with your GP or specialist to weigh the options.
Heavy Alcohol Consumption and Substance Abuse
Chronic alcohol abuse affects bone density and immune function similarly to smoking. Heavy drinkers often have nutritional deficiencies that hinder healing. Furthermore, post-operative care requires strict adherence to hygiene protocols. If substance abuse interferes with your ability to maintain oral hygiene or attend follow-up appointments, the risk of failure becomes too high for any ethical practitioner.
Pregnancy and Hormonal Changes
If you are pregnant, elective surgeries like dental implant placement are postponed until after childbirth. The hormonal changes during pregnancy increase gum sensitivity and bleeding risk, while the stress of surgery is unnecessary for both mother and baby. Additionally, taking X-rays and certain antibiotics or painkillers is restricted during pregnancy. It’s not that you’re permanently ineligible, just temporarily paused.

Psychological Factors and Expectations
Sometimes, the barrier isn’t physical but psychological. Patients with unrealistic expectations-such as expecting perfect symmetry or immediate results without understanding the healing timeline-are often advised against proceeding. Dental anxiety can also be a factor. If you cannot sit still for a procedure that lasts several hours, or if you suffer from severe gag reflexes that cannot be managed with sedation, the surgery may not be feasible.
Age Considerations
You must be physically mature before getting implants. Children and teenagers whose jaws are still growing are not candidates. Placing a fixed titanium post in a growing jaw can result in the implant appearing sunken as the surrounding bone continues to develop. Most surgeons wait until patients are at least 18, and often older, to ensure growth is complete. Conversely, age itself isn’t a disqualifier for older adults, provided their health is good.
| Factor | Status | Action Required |
|---|---|---|
| Bone Density | Insufficient | Bone grafting required or consider alternatives |
| Diabetes | Uncontrolled (HbA1c > 8%) | Stabilize blood sugar levels first |
| Smoking | Current smoker | Quit smoking for at least 2 weeks pre/post-op |
| Medications | IV Bisphosphonates | Consult specialist; likely ineligible |
| Age | Under 18 | Wait until jaw growth is complete |
Alternatives When Implants Aren't an Option
If you fall into one of these categories, don’t despair. You still have options to restore your smile and function. Dental bridges, which fixed prosthetic teeth anchored to adjacent natural teeth, are a common alternative, though they require grinding down healthy neighboring teeth. Partial dentures, which are removable appliances that replace one or more missing teeth, offer a non-invasive solution. For full mouth restoration, All-on-4, a technique using four strategically angled implants to support a full arch of teeth, sometimes viable even with less bone, might be explored with a specialist, though it still requires adequate bone quality.
Can I get dental implants if I have gum disease?
Not immediately. Active periodontal disease (gum disease) must be treated and controlled before implant placement. Bacteria from gum disease can spread to the implant site, causing infection and failure. Your dentist will likely recommend deep cleaning and possibly antibiotics first.
Are dental implants covered by the NHS in the UK?
Generally, no. The NHS considers dental implants cosmetic and rarely funds them unless there are exceptional clinical circumstances, such as trauma or congenital defects. Most patients pay privately, with costs ranging from £2,000 to £5,000 per implant depending on location and complexity.
How long does bone grafting take before I can get an implant?
Bone grafting typically requires 3 to 6 months of healing time before the implant can be placed. This allows the new bone to integrate and strengthen sufficiently to support the titanium post. Some advanced techniques may shorten this timeline, but patience is key for success.
Does smoking always mean I can't have implants?
It doesn't always mean no, but it makes it very risky. Many surgeons will only proceed if you commit to quitting smoking for a specific period before and after surgery. If you continue to smoke heavily, the likelihood of implant failure increases dramatically, making you a poor candidate.
What if I have osteoporosis? Can I still get implants?
Mild osteoporosis is often manageable, but severe cases or those treated with intravenous bisphosphonates are high-risk. Your dentist will coordinate with your GP to assess your bone density and medication history. In some cases, alternative treatments like bridges may be safer.